Therapeutic laser devices have been used worldwide for more than twenty years, but only recently has this technology begun to be integrated into routine medical practice on a larger scale. Technological and manufacturing innovations have made laser devices affordable while providing sufficient power to enable comprehensive therapy in a reasonable time. With increasing studies, we are finding that therapeutic lasers are effective in treating many disorders.
The photochemical effect in the target cell occurs after absorption of laser light by chromophores (the light-absorbing part of the cell). Photobiomodulation, as scientists have aptly named this phenomenon, is an example of a photochemical process in which photons emitted from a laser source act on target cells and induce stimulatory or inhibitory biochemical changes.
There are more than 3,000 published studies on non-ablative laser therapy. Many of these studies have been conducted on cells in vitro and have shown convincing results regarding the effect of laser light on various cell types. They have demonstrated increased angiogenesis, neurite extension, normalization of ion channels, cell membrane stabilization, and many other cellular changes.
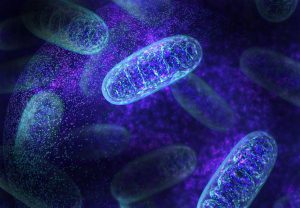
The exact mechanism of action of photobiomodulation is still being discussed in the scientific community. Several mechanisms are likely involved depending on the type of cell being stimulated. The most supported mechanism to date is that cytochrome C, located on the inner membrane of the mitochondria, acts as a photoreceptor. Cytochrome C absorbs light from 500 nm to 1100 nm due to the specific properties of this large molecule. Once light is absorbed, cytochrome C becomes excited, allowing it to bind more easily with oxygen and become cytochrome C oxidase, a compound critical for ATP formation. ATP is the activated energy carrier in the cell and facilitates many biological reactions or secondary mechanisms. These cellular mechanisms initiate pain reduction, inflammation reduction, and tissue healing.
Cells and biological tissue respond to light across a wide range of wavelengths, from ultraviolet to near-infrared. Choosing the correct wavelength ensures that light penetrates through skin, fat, and muscle to the treated target cells. Biological tissue either reflects, absorbs, scatters, or transmits light. The primary chromophores in tissue relevant to laser therapy application are hemoglobin, oxyhemoglobin, water, and melanin.
When deep-penetrating photobiostimulation occurs, pain relief, inflammation reduction, and accelerated tissue healing result. The best clinical outcomes are achieved when a sufficient number of photons penetrate the target tissue. The therapeutic dose is measured in joules (J) delivered per cm².
It has been demonstrated that tissues that are ischemic due to inflammation, swelling, and damage show significantly higher response to laser light than normal tissues. The biological response to photon flooding includes DNA/RNA synthesis, increased cAMP levels, protein and collagen synthesis, and cell proliferation. These reactions lead to rapid normalization, regeneration, and healing of damaged tissue – laser light modulates cellular metabolism.
Absorption of laser light energy by skin and subcutaneous tissue is estimated at 50–90%, with absorption increasing along with increasing wavelength. Longer wavelengths up to approximately 1000 nm are advantageous for deeper penetration, which initiates pain and inflammation relief and accelerated healing. Light penetration into tissue is key to therapeutic outcomes, and longer wavelengths lead to deeper penetration.